When young people turn 18, a lot happens. For instance, in Washington State, 18 is the age when a person legally becomes an adult and must handle tasks and make decisions that used to be made for them by adults.
Adult responsibilities and decisions can feel scary and confusing for the unprepared. Becoming responsible for medical care is part of growing up, and that process is so critical that there’s a specific name for it: healthcare transition.
For example, at age 18, a young adult is responsible for signing official paperwork to authorize procedures or therapies and to pay for co-pays. They must sign documents stating who can look at their medical records, speak with their doctors, or attend an appointment with them. Those rules are part of HIPAA, which stands for the Health Insurance Portability and Accountability Act. HIPAA is a federal law that protects confidentiality, regardless of disability. In this video, young adults living with various disabilities and medical conditions share their journeys through the adult healthcare system. They talk about how they make decisions and how they ask for help. Their ability to explain their needs, make decisions, and speak up for themselves is called self-advocacy. Take a look and listen to what they have to say in their own words!
Learning these skills isn’t something that happens the minute you turn 18. It takes practice to learn how to ask questions at the doctor’s office, to remember to ask about medications, to bring your insurance card. If you are a youth or young adult, those are things you can start early. If you are a caregiver or parent, begin giving your young adult or child questions to ask the doctor when they go in for well-child checks at age 12 or 13. Start talking with them about the conditions they may have and answer any questions they have honestly. If they are aware of why their body is doing what it is doing they can better manage their needs and ask for help when they need it. Help them learn to manage medicine with medicine reminder apps and pill containers. These kinds of things not only set them up for success when they are 18 at the doctor’s office, but also helps them advocate better for what they need in school and the community.
Here are some great sites that provide comprehensive step by step guidance to this process. See what fits best for yourself as a young adult; parents and guardians can think about what fits your family from their point of view.
- Got Transition has great tools and videos for youth, families, and providers. Young adults and families developed it, so it is peer-based.
- Charting the LifeCourse™ was created by families to help individuals and families of all abilities and all ages develop a vision for a good life, including their health care.
- The Center for Transition to Adult Health Care for Youth with Disabilities is a national health care transition resource center. The goal of the center is to empower youth and young adults with intellectual and developmental disabilities (ID/DD), ages 12-26, to direct their own transition from pediatric to adult care, with no reduction in quality of care and no gaps in services.
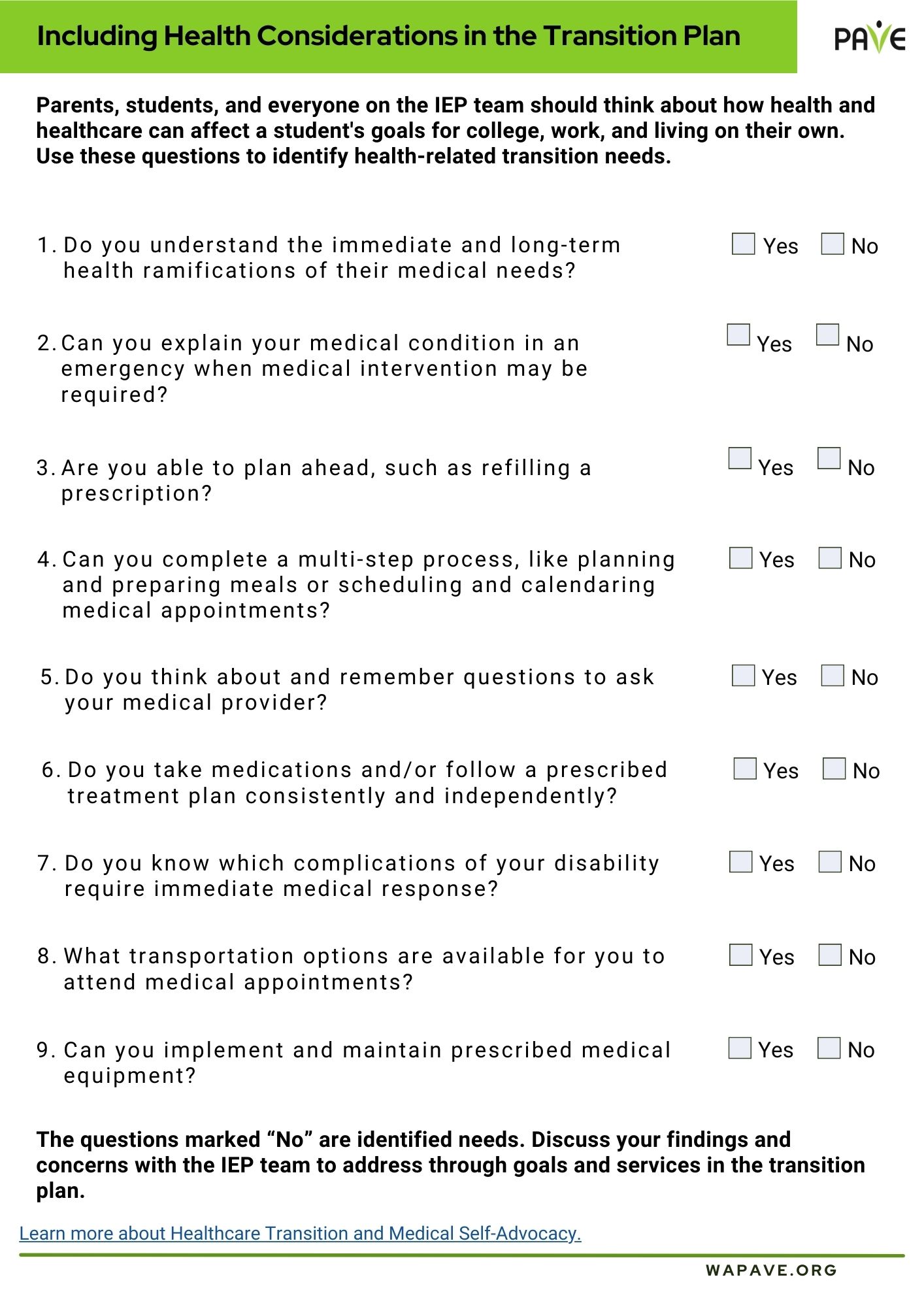
Including Healthcare Needs and Goals in the Transition Plan
Healthcare transition is often left out of the transition process and left to parents and students to do themselves. Parents, students, and everyone on the IEP team should think about how health and healthcare can affect a student’s goals for college, work, and living on their own. Parents and students can ask that this be a part of the transition plan and can use the resources listed above in the planning process.